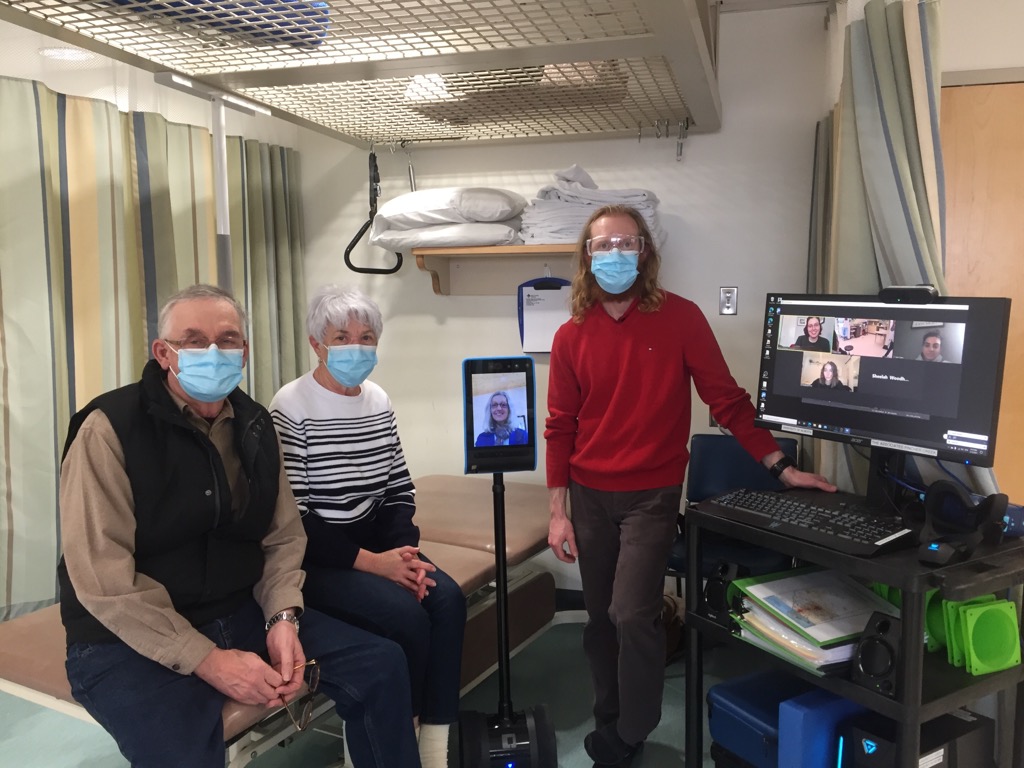
Crowsnest Pass residents requiring additional rehabilitation support are now able to remotely access expertise from larger centres thanks to a cutting-edge technology project funded through RhPAP.
Dubbed Tele-Rehabilitation 2.0, the program—offered by the University of Alberta’s Faculty of Rehabilitation Medicine Project—features remote control robots, motion-capture equipment to pinpoint patient body activities, video monitoring, and more. RhPAP provided $15,000 to the Crowsnest Pass Health Centre in Blairmore to link to the system in late 2020.
Tele-Rehab 2.0 was born out of the reality that most of Alberta’s expert or experienced clinicians congregate in urban centres, while a quarter of the province’s population lives rurally with travel to cities presenting a barrier to care for rural patients.
“This is Canada. This is the 21st century. This is unacceptable,” said Emily Armstrong, the project coordinator. “We developed Tele-Rehab 2.0 as a model to help bridge that gap.”
Armstrong says the project supports rural clinicians who can feel isolated. They’re generally the only physiotherapist in the community and are often new graduates.
“[Local clinicians now] feel really involved in the discussion and included, and they’re ‘upskilling,’ and they’re getting questions answered,” said Armstrong.
“We really want virtual care to be comparable to face-to-face care.”
– Emily Armstrong, project coordinator
Tele-Rehab 2.0 connects expert clinicians with local patients and their local clinicians via telehealth–health-care remotely aided by telecommunications. This program uses telepresence robots, motion capture, vestibular goggles (diagnostic infrared goggles that let the hub clinician get a good look at a patient’s eyes), and video recording for later playback.

– Photo supplied by University of Alberta’s Faculty of Rehabilitation Medicine Project Tele-Rehab 2.0.
Through this technology, the remote clinician is able to drive a telepresence robot, aided by a camera and a screen that gives them the view they need to assess patients.
Kinetisense, a Medicine Hat-based company, created the markerless motion-capture software, which requires no markers or special clothing to be worn by the participant. Kinetisense captures kinematic data of movements of all kinds including range of motion, gait, sway when balancing, wheelchair propulsion movements, and functional mobility (like moving from sitting to standing position). The data helps the clinician assess and track progress of patients in a less tedious manner than conventional methods.
Martin Ferguson-Pell, professor at the University of Alberta Faculty of Rehabilitation Medicine and a biomedical engineer, founded Tele-Rehab 2.0 in 2019 after receiving a grant from Alberta Innovates.
Ferguson-Pell said the development of small, inexpensive technologies to make measurements with more affordable sensors, and the emergence of Alberta-based Kinetisense contributed to an “a-ha” moment when his team “realized that we were in a very strong position to start to create this platform.
The small team of three was ready to roll out community trials in March 2020 when COVID-19 struck. It was delayed until June 2020, when Ferguson-Pell could deliver the equipment to the rural communities.
Ferguson-Pell said delivering the equipment was “one of the most satisfying things you could imagine” as it created an alternative to travelling to a city for rural patients.
“Especially in the winter, [travel] is extremely dangerous,” he said, noting the loss of Greyhound bus services in 2018 left vulnerable rural Albertans even more remote.
Tele-Rehab 2.0 currently focuses on four areas of treatment: vestibular care (vertigo), severe shoulder pain and instability, custom wheelchair seating, and hip and knee surgery follow-up appointments.

– Photo supplied by University of Alberta’s Faculty of Rehabilitation Medicine Project Tele-Rehab 2.0
Armstrong is particularly excited about treating vertigo.
“We’ve helped [about] 10 people in the last year just get back to normal life,” said Armstrong.
Taking into account the other areas of treatment, Ferguson-Pell estimates about 50 patients have been treated through the program so far, including those at continuing care facilities in Edson, Hinton, and Grande Cache.
Future work through Tele-Rehab 2.0 may include treatment of stroke spasticity (muscles become stiff and resist stretching after a stroke), lymphedema (swelling in arms or legs often related to damage or removal of lymph nodes in cancer treatment), and fall-risk assessments for health-care facilities.
They would also like to utilize monitoring systems for patients at home to help them reduce travel even further.
“The world is our oyster,” said Armstrong.
The impact of COVID-19 actually helped Tele-Rehab 2.0 gain traction, as health professionals were forced to adopt virtual care.
“We really want virtual care to be comparable to face-to-face care,” said Armstrong.
Ferguson-Pell added: “We’re not claiming that what we’re doing is covering every clinical eventuality, but what we’re wanting to do is at least reduce the number of trips it’s necessary for people to make.”
The pilot project—with further funding from AHS—will see 10 more systems added across rural Alberta in addition to Blairmore.
Tele-Rehab 2.0 also has equipment in Peace River, Pincher Creek, and Jasper.
More information on the impact of this program can be found at telerehabilitationcollaboration.com.
